If you’ve been asking whether an NEMT business can still turn a real profit in 2026, the answer is yes — but the “how” matters enormously. Demand remains strong, but margins are tighter, operations are more complex, and success depends heavily on how the business is run. This article breaks down what the NEMT market is today, the real challenges facing transportation providers this year, and the proven strategies that make NEMT services profitable despite mounting headwinds.
What is NEMT?
Non-Emergency Medical Transportation (NEMT) is a federally mandated benefit under Medicaid that provides scheduled rides to medical appointments for patients who need assistance but are not in an emergency. Unlike ambulance services, NEMT supports routine and recurring healthcare needs, including dialysis, behavioral health visits, primary care, and physical therapy. For many patients—particularly those managing chronic conditions—these trips are not optional. Missing appointments can lead to worsening health outcomes and higher downstream costs for the healthcare system.
How Big Is the NEMT Market in 2026?
According to 360iresearch, the global NEMT market was estimated at USD 18.19 billion in 2026 and is projected to reach USD 25.43 billion by 2032, growing at a CAGR of 5.52%. North America holds the largest regional market at 40-45%.
What drives this growth? Three unstoppable forces:
- An aging population. Adults aged 65+ spend nearly 3.5 times more on healthcare annually compared to those ages 18–64. Today there are approximately 61.2 million Americans in this age group. By 2030, that number is expected to increase significantly, with nearly 1 in 5 Americans over the age of 65. In some states and metro areas, older adults are outnumbering children for the first time—a shift that signals long-term demand for healthcare services, including transportation.
- Chronic disease prevalence. Chronic and mental health conditions account for roughly 90% of the nation’s $4.9 trillion in annual healthcare spending. These conditions often require frequent, ongoing care. For example, dialysis patients typically require transportation three times per week—totaling more than 150 trips annually per patient.
- Medicaid Utilization Density. While total Medicaid enrollment may stabilize or slightly decline due to policy changes and eligibility redeterminations, frequent and consistent care is still needed for those remaining on Medicaid. Which makes transportation a necessary determinant to managing their health outcomes.
The Real Challenges Facing NEMT in 2026
Despite the continued growth of the NEMT market, margins across the industry are under pressure from rising costs, policy changes, labor constraints, and operational complexity. This is reflected more broadly across the transportation sector, where data from the Bureau of Labor Statistics shows that 20-25% of new entrants do not make it past their first year. The common challenges are:
1. Rising Operational Costs
Maintaining competitive pricing while managing rising costs is one of the biggest challenges providers face. Increased litigation and claims, higher risk exposure for larger vehicles and fleets, rising repair costs for specialized vehicles, and stricter compliance standards have all contributed to higher commercial auto insurance premiums. At the same time, vehicle costs have increased—driven in part by tariffs and fuel price volatility—while driver wages continue to rise. Despite these increases, Medicaid reimbursement rates in many states have remained relatively flat. This growing imbalance between cost and revenue is one of the most pressing threats to profitability in 2026.
2. Driver Shortages and Turnover
Recruiting and retaining qualified drivers remains a persistent challenge. Some transportation providers report high levels of turnover due to the demanding nature of the role. NEMT drivers must meet strict requirements, including specialized training (such as wheelchair securement), HIPAA awareness, and background checks, which narrows the available labor pool. In addition, the role can be physically and emotionally demanding, while wages often struggle to compete with other transportation and gig economy opportunities. Together, these factors make workforce stability difficult to maintain.
3. Regulatory Changes
Ongoing Medicaid cost-containment efforts are introducing additional complexity for transportation providers, with states tightening reimbursement structures, authorization requirements, and utilization oversight. These policy shifts can directly impact both margins and trip volume. As a result, providers are expected to operate more efficiently while meeting increasing compliance and reporting demands.
4. Claim Denials and Cash Flow Gaps
Medicaid brokers typically take 30–90 days to pay after service delivery, with 10–20% of claims initially denied. These delays create financial strain, particularly for smaller or undercapitalized operators, limiting their ability to scale even when demand is strong.
How NEMT Transportation Can Still Be Profitable in 2026
Despite these headwinds, the fundamentals for NEMT transportation profitability remain strong if operators implement the right strategies.
Specialized transportation
The revenue potential for specialized service is significantly higher although rates vary significantly by state, payer, and contract structure. In many markets, this translates to approximate ranges such as:
- Ambulatory Trips: Base rate of $10–$25 plus a low mileage fee ($1.00–$1.50).
- Wheelchair Trips: Generally command a base rate of $35–$65 with higher mileage modifiers ($2.00–$3.50), reflecting the specialized equipment and securement training involved.
- Stretcher Trips: These represent the highest tier of NEMT, with base rates typically ranging from $125 to over $250, as they require dual-staffing and heavy-duty vehicles.
Because fewer providers are equipped to deliver wheelchair and stretcher services, these segments often face less competition while serving patients with more consistent and recurring transportation needs.
Leverage Route Optimization and NEMT Scheduling Technology
Route optimization and NEMT scheduling software are the single biggest levers available to NEMT operators in 2026. Low vehicle utilization remains a persistent challenge across NEMT. Research from the GAO and the FTA highlights inefficiencies in routing, scheduling, and network coordination that lead to underutilized vehicles and excess mileage. Advanced platforms can save providers 2–3 hours of administrative work per day by automating scheduling, dispatching, and trip management. In addition, route optimization and dynamic scheduling improve fleet utilization, reduce deadhead miles, and increase trips completed per vehicle—ultimately boosting monthly revenue without requiring additional vehicles or drivers.
Build a Diversified Payer Strategy
Expanding beyond traditional brokered Medicaid trips is critical, as relying on a single revenue source limits margin potential. Diversification helps offset reimbursement constraints, improves revenue stability, and reduces financial risk.
- PACE programs: Contracting directly with PACE organizations creates opportunities beyond traditional transportation services. In addition to transporting participants, providers can support services such as meal delivery, medical supplies, and prescription transport. While this model requires closer coordination, it offers more predictable demand and a steady, recurring flow of trips.
- 1915(c) waiver programs (HCBS): Although still Medicaid-funded, these programs are tied to long-term services and support (LTSS). They create access to non-traditional trip types, including community-based transportation, which can be less competitive than standard brokered volume.
- Private-pay and facility-based contracts: These models provide greater control over pricing and payment timelines, allowing providers to improve margins and reduce dependency on fixed reimbursement rates.
- Supplemental benefit programs: Medicare Advantage plans and D-SNPs can offer more flexible reimbursement structures. While some plans have scaled back transportation offerings following pandemic-era expansions, these benefits remain available creating alternative contracting opportunities.
Prioritize Recurring, High-Frequency Trips
Recurring trips are one of the strongest drivers of operational stability and profitability in NEMT. These trips are easier to plan, optimize, and staff—making them more efficient to deliver at scale.
- Focus on repeat services such as dialysis, behavioral health, and ongoing care
- Build schedules around predictable, high-frequency demand
- Improve route density and reduce variability in daily operations
Patients with chronic kidney disease, particularly those with end-stage renal disease (ESRD), are among the highest utilizers of NEMT services. In 2018, they averaged 70.1 ride days per year, reflecting consistent and recurring transportation needs. Private dialysis transport can generate $75–$150 per trip compared to Medicaid rates of $40–$60, with a single patient contributing nearly $12,000 in annual revenue.
Behavioral health transportation is also expanding rapidly. As one of the fastest-growing segments in NEMT—projected to grow at a 9.55% CAGR (Mordor Intelligence)—it presents an opportunity for providers to access higher-value trips while meeting increasing demand driven by broader behavioral health coverage and parity initiatives.
Target High-Growth Niches
The NEMT segments with the highest growth rates according to Mordor Intelligence are:
- Mental health transportation — 9.55% CAGR
- Dialysis — 5% CAGR
- Routine doctor visits — 4.2% CAGR
- Diagnostic or therapy visits — 9% CAGR
Providers who position early in mental health and home healthcare transport face less competition while riding the fastest-growing demand curves.
Optimize Billing and Reduce Denials
Across the US, 10–20% of Medicaid NEMT claims are denied on first submission (CMS), creating 30-90 day delays, rework, and unrecoverable revenue. For example, a 15% claim denial rate on $1 million in revenue means $150,000 left on the table annually. Implementing automated billing systems and clean-claim protocols can cut denial rates to under 5%, dramatically improving cash flow without adding a single vehicle. Additionally, automation can shorten the reimbursement cycles to fewer than 30 days.
Highlight Your Performance to Prove Value
As healthcare shifts toward value-based models, NEMT will also be evaluated based on how it supports outcomes—not just whether a trip was completed. To stay competitive, providers should build and structure their data around the KPIs that matter most to payers—tracking performance in a way that aligns with how payer contracts are evaluated and decisions are made.
For example, use technology to track KPIs that directly impact health outcomes and reduce costs:
- On-time performance (OTP): Late arrivals lead to missed or delayed appointments–big cost drivers to healthcare costs.
- Missed trips / no-shows: Track both provider-driven and member-driven no-shows; both impact care continuity
- Member experience metrics: Track member complaints, call wait times, response rates, resolution timelines. These indicators reflect service quality and are frequently used to evaluate broker performance and member satisfaction.
Profitability Benchmarks: What Can You Realistically Earn?
With the right strategies, here is what NEMT business owners can realistically expect:
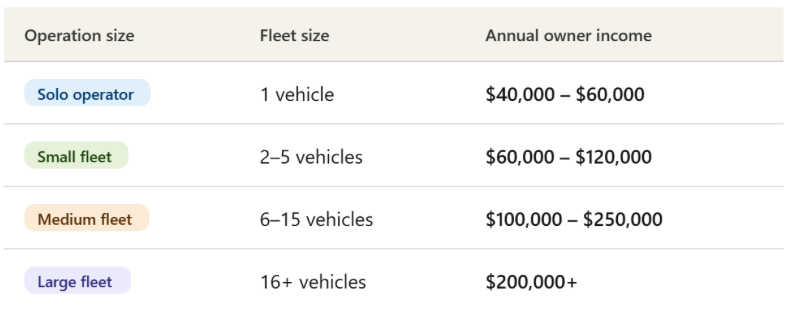

Source: Elite Med Financials
Profit margins by service type range from 15–25% for ambulatory transport to 20–30% for wheelchair and stretcher services. These margins are achievable, but only with technology adoption, clean billing, and diversified payer mix.
The Bottom Line: Is NEMT Transportation Worth It in 2026?
NEMT transportation in 2026 is not a passive income play. Rising costs, driver shortages, and compliance demands are real. But the underlying demand, driven by demographics, Medicaid mandates, and healthcare’s recognition of transportation as a social determinant of health, is irreversible.
Every $1 invested in NEMT services generates $11 in healthcare savings (Florida State University). Operators who adopt NEMT software, diversify their payer mix, target high-growth niches like mental health, and master billing will find that non-emergency medical transportation (NEMT) remains one of the most durable, mission-driven businesses in healthcare today.
About Move AI
Move AI is rideshare-grade orchestration for NEMT. It gives brokers and transportation providers the freedom to grow by handling the nuances of every trip with built-in speed, precision, automation, and compliance.